Connections & integrations
Loading...
Loading...
December 2020
November 2020
Command Center
Date of birth mismatches added to Reconciliation
API
API support for COBRA enrollments
October 2020
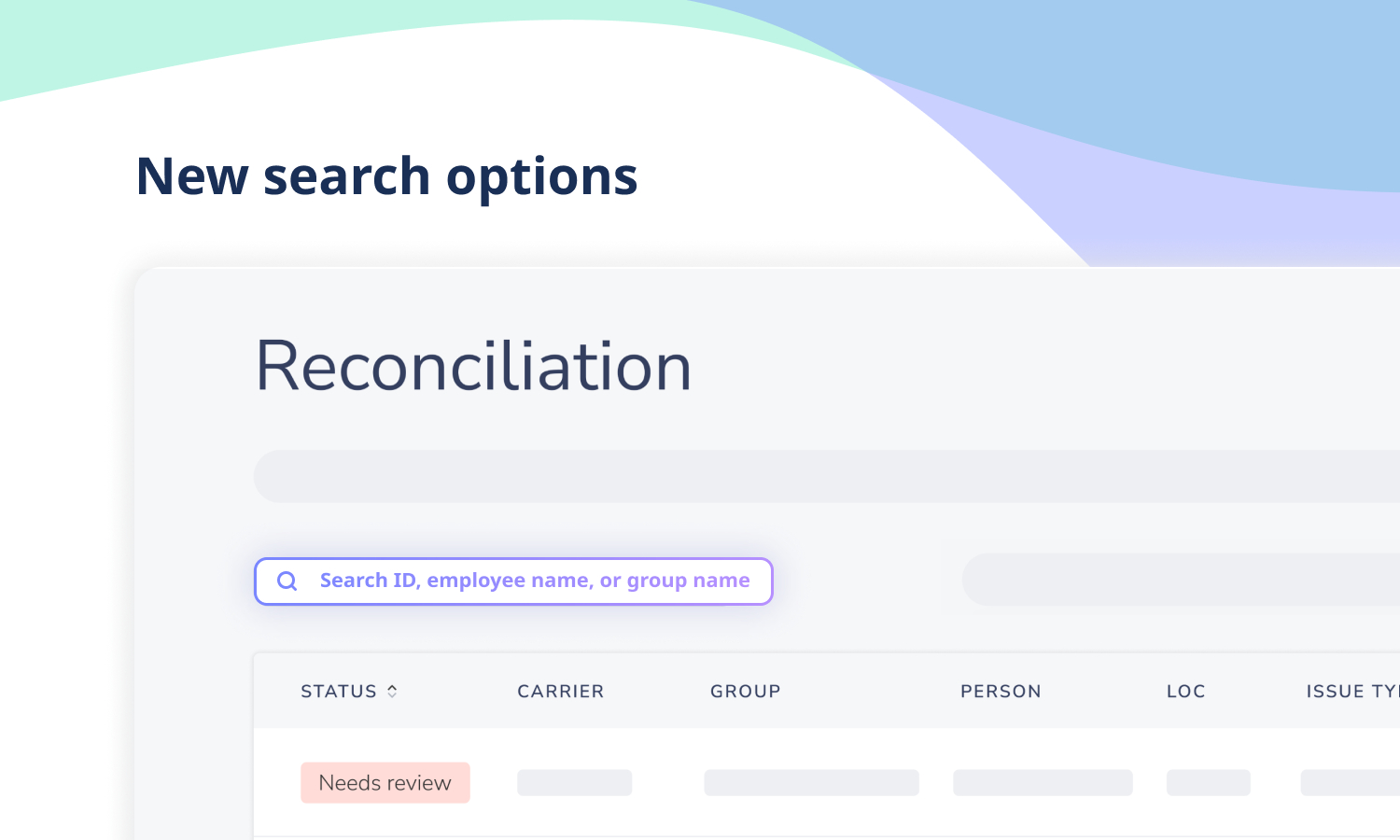
Command Center
Expanded search capabilities for requests
API
New endpoint for member premiums
September 2020
Connections & integrations
Company news
Announcing our Series A and new partnerships
API
More flexibility for new hire enrollments
API
Support for accident and critical illness plans
August 2020
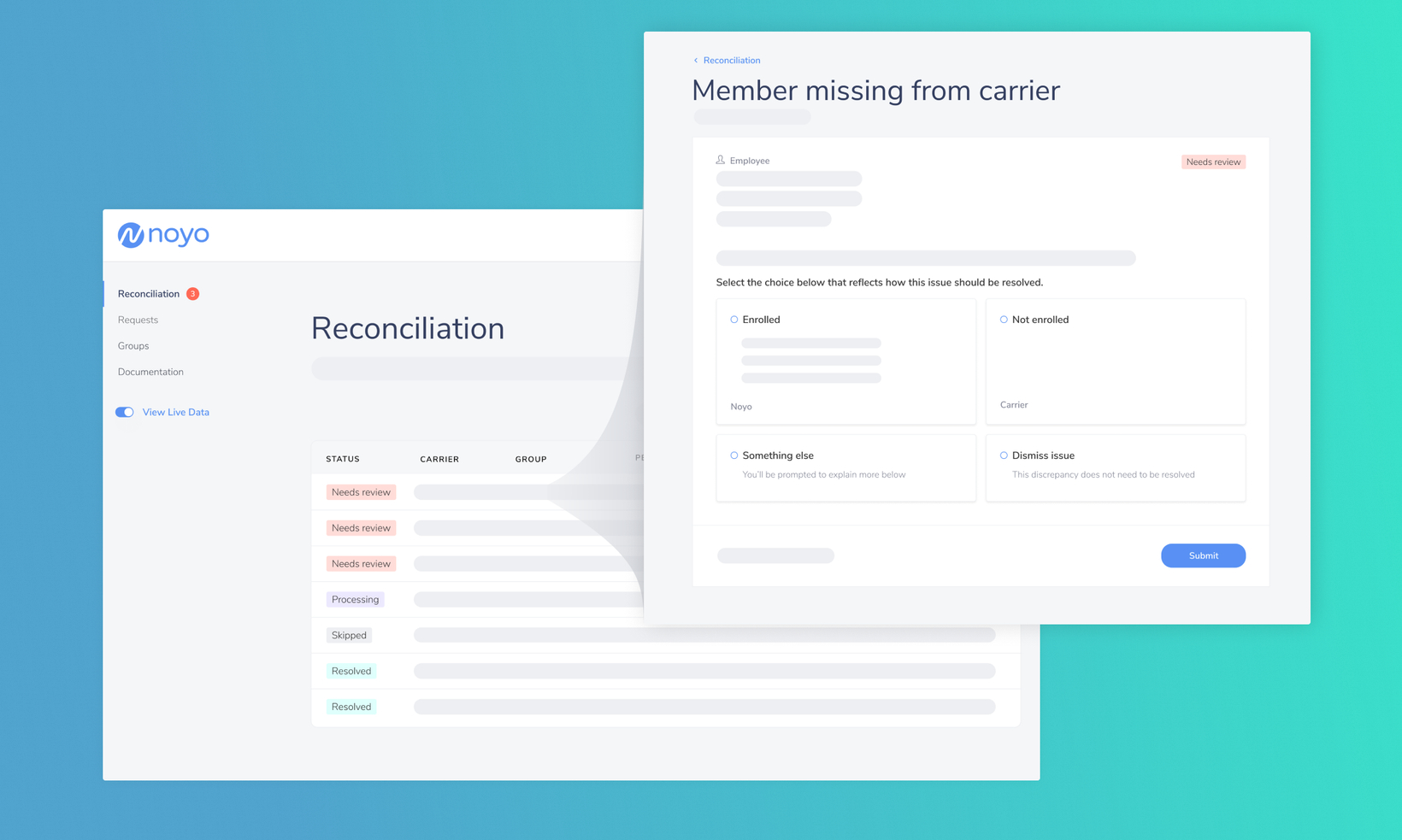
Command Center
Reconciliation: A powerful new tool for benefits administration platforms
API
Map groups and find records faster
- Jump to Month
- March 2025
- October 2024
- September 2024
- July 2024
- May 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- February 2023
- December 2022
- October 2022
- August 2022
- April 2022
- March 2022
- January 2022
- November 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020